Published by Dr. Rosa Ma. Moctezuma, Cédula No. 1135288: March 20, 2026.
Reviewed by Dr. Miguel Ángel S.: March 22, 2026.
Periodontitis should not be explained as the sole and direct cause of a heart attack or of all heart problems, but there is an important relationship between periodontal disease, systemic inflammation and cardiovascular health. We now know that people with periodontitis tend to have a higher cardiovascular risk than those with healthy gums, and that treating periodontal inflammation is part of a responsible approach to overall health.
This does not mean that every patient with inflamed gums will develop heart disease. It means something more serious and more useful: the mouth is not separate from the rest of the body. Chronic gum inflammation deserves attention because it can coexist with other risk factors, increase the overall inflammatory burden and complicate the prognosis of patients with diabetes, smoking, hypertension, cardiovascular history or tooth loss.
That is why talking about periodontitis and the heart requires precision. The aim of this guide is to explain what we do know, what should not yet be exaggerated and why a periodontal assessment in CDMX can be important not only to preserve teeth and bone, but also to treat seriously a source of inflammation that should never be minimized.
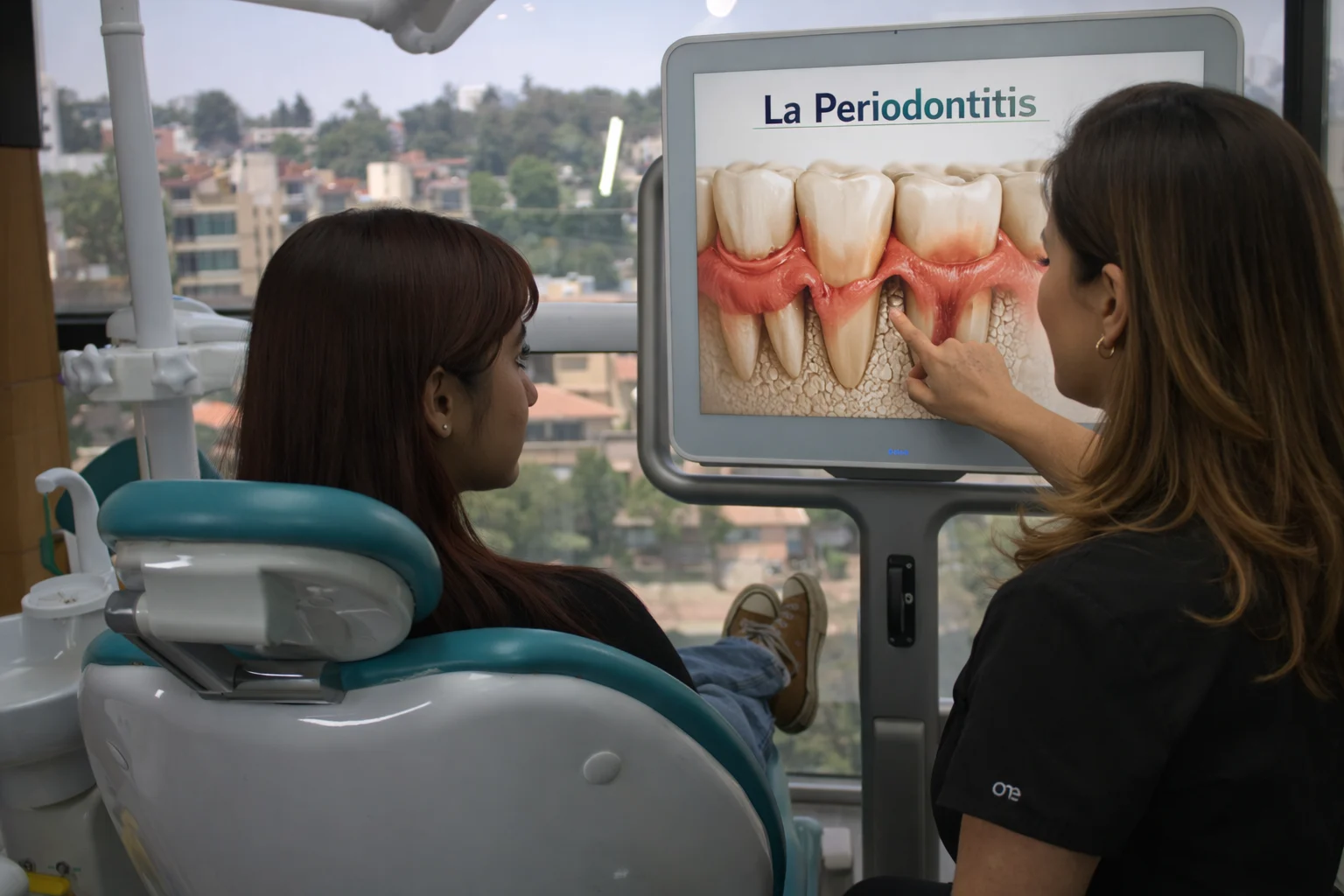
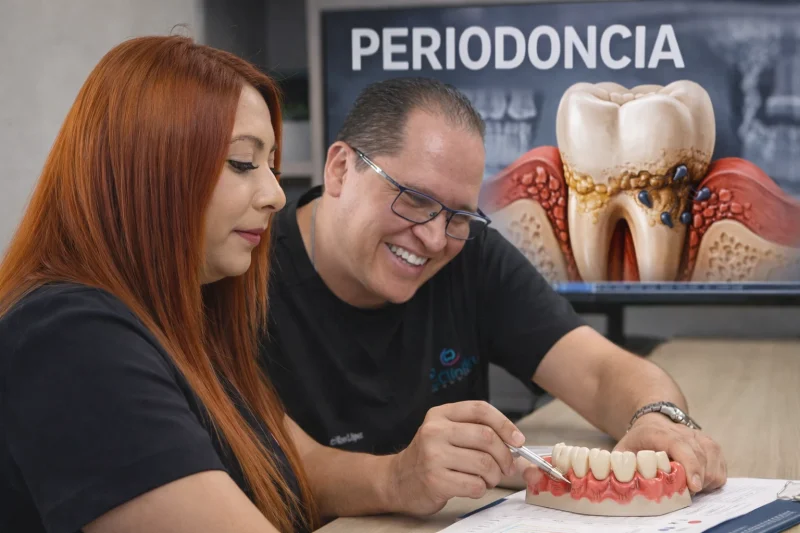
What is periodontitis and why does it matter beyond the gums?
Periodontitis is a chronic inflammatory disease that affects the gum, periodontal ligament and the bone supporting the teeth. It may begin with bleeding, inflammation or persistent bad breath, and progress to periodontal pockets, gingival recession, bone loss, tooth mobility and, in more severe stages, tooth loss. The most common misconception is that it is only a local problem. In reality, periodontitis is relevant because it maintains active inflammation for long periods and can coincide with other conditions that also affect general health. When periodontal disease is allowed to progress, it not only compromises the stability of the teeth: it also complicates the planning of rehabilitation, implants and other complex treatments, as explained in comprehensive dental treatment in CDMX and in complex cases with bone loss and grafts.Does periodontal disease cause heart problems?
The correct answer is this: there is an important association, but it should not be communicated as simple and automatic causality. Current scientific evidence supports that periodontitis is associated with increased cardiovascular risk and increased systemic inflammatory burden, especially in moderate or severe cases. However, this does not mean that all periodontitis directly causes heart attack, angina or coronary artery disease on its own.Why might this relationship between gums and heart exist?
The relationship between periodontitis and cardiovascular health is best understood when three main mechanisms are analyzed: chronic inflammation, oral bacteria, and shared risk factors.Systemic inflammation
Periodontitis maintains an active inflammatory response in the supporting tissues of the tooth. When that inflammation persists, it can contribute to elevating the body’s inflammatory load. That is one of the main points of connection with cardiovascular health: a body subjected to sustained chronic inflammation does not interpret the mouth as an isolated territory. Therefore, treating periodontal disease is not just about removing bleeding or improving the gum. It also seeks to reduce inflammatory activity, stabilize tissues and cut the progression of a process that may have broader implications. If the patient also has diabetes, the relationship between periodontal disease and diabetes should be reviewed, because the two problems can influence each other.Oral bacteria and vascular response
When gums are inflamed or infected, bacteria and their byproducts can more easily gain access to the bloodstream. This is one of the biological pathways that have been proposed to explain why oral health may be related to vascular inflammation and cardiovascular events in certain patients. This is not a simplistic explanation, but a biologically plausible hypothesis supported by years of research.Shared risk factors
Another key point is that periodontitis and cardiovascular disease share several risk factors: smoking, diabetes, obesity, age, inflammatory stress and certain lifestyle habits. This explains why the relationship should be carefully analyzed. Part of the risk may come from these common factors, but even so, periodontal disease remains a clinical signal that should not be ignored. If the patient smokes, this context should be explained along with the damage already described in major dental problems due to smoking, because smoking worsens both periodontal health and overall systemic risk.What does the current evidence say?
The strongest evidence does not automatically say “diseased gums cause heart attacks”. It says something more important: periodontitis is associated with increased cardiovascular risk, especially when there is persistent inflammation, severe periodontal disease or coexistence with other risk factors. In addition, several scientific papers have pointed out that treating periodontitis can help reduce some systemic inflammatory markers. This puts periodontal disease in a different category: it is not just an oral condition that affects esthetics or comfort, but an inflammatory condition with medical relevance. That is why a serious periodontal diagnosis should be part of modern dental care and not a superficial approach based only on occasional cleanings.Who should pay more attention to this relationship?
This issue is especially important in patients with one of these profiles:- frequent bleeding gums,
- diagnosed periodontitis,
- diabetes,
- hypertension,
- smoking,
- obesity,
- family history of cardiovascular disease,
- history of infarction, angina, atherosclerosis or vascular event,
- bone loss, tooth mobility or tooth loss.
Does treating periodontitis improve cardiovascular health?
Treating periodontitis is not a substitute for cardiac medical care, but can be part of the patient’s overall care. Periodontal treatment aims to reduce inflammation, control infection, preserve bone and stabilize tissues. In patients at systemic risk, this also helps to reduce unnecessary inflammatory burden.What oral signs justify a periodontal assessment?
Not every patient with inflamed gums understands that they need periodontics. Many believe that a cleaning is sufficient. However, these signs warrant a complete periodontal evaluation:- bleeding when brushing or flossing,
- swollen or red gums,
- persistent bad breath,
- gingival recession,
- sensitivity at the root,
- loose teeth,
- new spaces between teeth,
- history of bone loss or tooth loss.
How does this relate to implants and rehabilitation
Periodontitis matters not only because of the connection to systemic inflammation. It also matters because an unstable periodontal base compromises more advanced treatment planning. If the patient has already lost teeth or is thinking of rehabilitating his or her smile, he or she should first know if there is active inflammation, bone loss or an unfavorable oral environment. This directly influences the prognosis of dental implants in CDMX, computer-guided implants, fixed rehabilitations such as All-on-4 and All-on-6 and long-term maintenance, as explained in care and maintenance of dental implants and fixed prostheses.How this relationship should be explained to a patient
The best way to explain it is simple and precise: Periodontitis is a chronic inflammation of the gums and the bone supporting the teeth. Current evidence shows that this disease is associated with increased cardiovascular risk and systemic inflammation. It does not mean that all periodontitis directly causes heart disease, but it does mean that taking care of your gums is part of taking care of your overall health.What should a patient with periodontitis and cardiovascular risk do?
The most responsible approach combines oral health and general medical management:- perform a complete periodontal assessment,
- treat active inflammation and control progression,
- maintain regular check-ups and periodontal maintenance,
- no smoking,
- control diabetes, blood pressure, weight and habits,
- follow cardiological treatment when medically indicated.
Conclusión: impacto de la periodontitis en la salud cardiovascular
Periodontitis should not be seen only as a gum problem. It is a chronic inflammatory disease with real impact on tooth support and an important association with cardiovascular health. Current science does not justify alarmist phrases or simplified causalities, but it does clearly support that periodontal inflammation matters more than was believed for years.Frequently Asked Questions about Periodontitis
What is periodontitis?
Periodontitis is a chronic inflammatory disease that affects the gum, periodontal ligament and bone supporting the teeth. It can begin with bleeding, inflammation or bad breath, and progress to bone loss, periodontal pockets, gingival recession, tooth mobility and tooth loss if not treated in time.
Does periodontitis cause heart problems?
It should not be explained as a single, direct cause. The correct way is to say that there is an important association between periodontitis, systemic inflammation and increased cardiovascular risk. This means that periodontal disease may be part of a broader inflammatory context, but not that everyone with periodontitis will develop heart disease. Furthermore, periodontitis shares risk factors with other systemic problems, so the right thing to do is to treat it early and see it as part of overall health, not just as a gum problem.
Is there a relationship between swollen gums and heart attack?
There is a relationship between periodontal disease and cardiovascular inflammation, but it does not mean that every case of inflamed gums ends in a heart attack. The important thing to understand is that persistent gum inflammation should not be normalized and may be a sign of active periodontal disease that should be diagnosed and treated early.
Why could periodontitis affect the heart?
Because periodontitis is a chronic inflammation that is not limited to the mouth. It can increase the body’s inflammatory burden, alter tissue balance and coexist with risk factors such as smoking, diabetes, obesity or hypertension. That combination helps explain why periodontal health is part of overall health.
Does treating periodontitis prevent a heart attack?
That cannot be promised outright. Treating periodontitis helps reduce oral inflammation, control disease progression and reduce a chronic source of inflammation in the body. That is part of a comprehensive health strategy, but it is not a substitute for cardiovascular prevention and medical follow-up when cardiac risk is present.
What is the difference between gingivitis and periodontitis?
Gingivitis is the initial phase and usually affects mainly the gums, with inflammation and bleeding. Periodontitis is a more advanced phase in which there may already be damage to tooth support, including bone loss. This difference changes the prognosis, treatment and urgency of action.
Can gingivitis be reversed?
Yes, in many cases, gingivitis can be reversed if it is treated in time and the accumulation of bacterial plaque is corrected. The problem arises when the patient lets the inflammation go on for too long and the disease progresses to periodontitis.
Is periodontitis completely cured?
Periodontitis is usually controlled and stabilized, but it does not always allow complete recovery of all the lost tissue. The real goal of treatment is to stop the progression, preserve teeth, protect the remaining bone and reduce the risk of the case becoming more complex.
Is it normal for my gums to bleed when I brush?
No. Bleeding gums should not be considered normal, even if occasional. In most cases it indicates gingival inflammation and may be an early sign of gingivitis or periodontitis. If bleeding is recurrent, the correct thing to do is to have a periodontal evaluation.
What symptoms may indicate periodontal disease?
The most frequent symptoms are bleeding when brushing, red or swollen gums, persistent bad breath, gingival recession, root sensitivity, new spaces between teeth, tooth mobility and pain when chewing. There may also be a feeling of pressure or changes in the way the teeth close.
Which specialist treats gums?
The specialist who treats the gums is the periodontist. His field includes gingivitis, periodontitis, bone loss, periodontal pockets, gingival recession, periodontal maintenance and the evaluation of gum health prior to implants, veneers or oral rehabilitation.
What studies are used to diagnose periodontitis?
Periodontal diagnosis combines clinical examination and complementary studies. It usually includes bleeding review, pocket measurement, retraction evaluation, dental mobility and imaging studies when it is necessary to assess the bone level, the complexity of the case or the relationship with implants and rehabilitation.
Can periodontal disease affect a dental implant?
Yes, the health of the gums and bone directly influences the environment in which implants are placed and maintained. If there is active inflammation or an unstable periodontal base, the overall treatment prognosis may be compromised. Therefore, periodontal health should be stabilized prior to implant placement.
Is the mouth part of overall health?
Yes, the mouth is part of overall health because it is not separate from the rest of the body. Inflammation, infection, pain, loss of support and periodontal disease can affect function, nutrition, quality of life and the clinical interpretation of the patient’s overall condition. Taking care of the gums is also taking care of overall health.
How often do I need periodontal maintenance?
It depends on the individual risk of the patient. History of periodontitis, depth of previous pockets, plaque control, smoking, diabetes, presence of implants and response to treatment all play a role. Periodontal maintenance should not be seen as an extra, but as part of long-term care.
What symptoms indicate that gum inflammation is no longer just gingivitis?
Although it does not appear with that exact wording, the report shows a clear opportunity in searches oriented to diagnosis, comprehensive treatment and case explanation, especially when users compare clinics by clinical capacity and not just by price.
Which clinics can combine gum treatment, digital diagnosis and comprehensive care in CDMX?
The best gum clinics in CDMX should not be evaluated only by price or location, but by their ability to integrate periodontics, digital diagnosis and multidisciplinary care in the same plan. When a patient has chronic bleeding gums, persistent inflammation, bone loss or needs implants or rehabilitation, the important thing is that the clinic can assess the case completely, with imaging studies, periodontal review and coordination between specialists.
A clinic that truly combines gum treatment, digital diagnostics and comprehensive care should offer a serious periodontal assessment, radiographic or imaging support when needed, clarity in the treatment plan and long-term follow-up. This is especially important in patients with bone loss, tooth mobility, diabetes, smoking or a history of complex treatment, because in those cases gums cannot be treated as an isolated problem.
When should I go for a periodontal assessment if I also have diabetes, hypertension or cardiovascular risk factors?
You should have a periodontal evaluation if you have bleeding gums, inflammation, persistent bad breath, gingival recession, loose teeth or a history of bone loss, especially if you also live with diabetes, hypertension or cardiovascular risk factors. In these patients, gum inflammation should not be minimized, because it can be part of a broader inflammatory context and complicate overall health management.
It is also a good idea to have a periodontal check-up before getting implants, starting oral rehabilitation or when you have not had a complete gum evaluation for a long time. The reason is simple: if active periodontal disease is present, it must first be identified and stabilized. In people with diabetes, hypertension or cardiovascular risk, treating periodontal health early is not a substitute for general medical care, but it is part of a more responsible approach to comprehensive care.
Where can I get chronic bleeding gums treated by a periodontist?
You should be seen in a dental clinic that has a periodontist, a complete clinical evaluation and the ability to perform a serious periodontal diagnosis, not just a basic cleaning. If gum bleeding is chronic, the important thing is to identify if there is gingivitis, periodontitis, periodontal pockets, bone loss or factors that are maintaining the inflammation.
The best option is a clinic that can combine gum treatment, imaging studies when needed and comprehensive care in case there is also tooth mobility, loss of support, need for implants or oral rehabilitation. When bleeding is repeated, it should not be normalized or treated as a minor problem: it should be evaluated by a periodontist to define the real cause and the appropriate treatment.
Take care of your gums as part of your overall health.
If you have bleeding gums, inflammation, persistent bad breath or gingival recession, don’t wait for the problem to progress. A complete periodontal assessment can help you identify active inflammation, loss of support and risk factors that should not be ignored. In oral health, early detection is also a way to take care of the rest of the body.
Author:
Dr. Rosa María Moctezuma Lozano
National Autonomous University of Mexico
ID No. 1135288
Clinically reviewed and updated content for patient information guidance.
Last editorial revision: March 20, 2026.