Published by Dr. Rosa Ma. Moctezuma, Cédula No. 1135288: March 20, 2026.
Reviewed by Dr. Miguel Ángel S.: March 22, 2026.
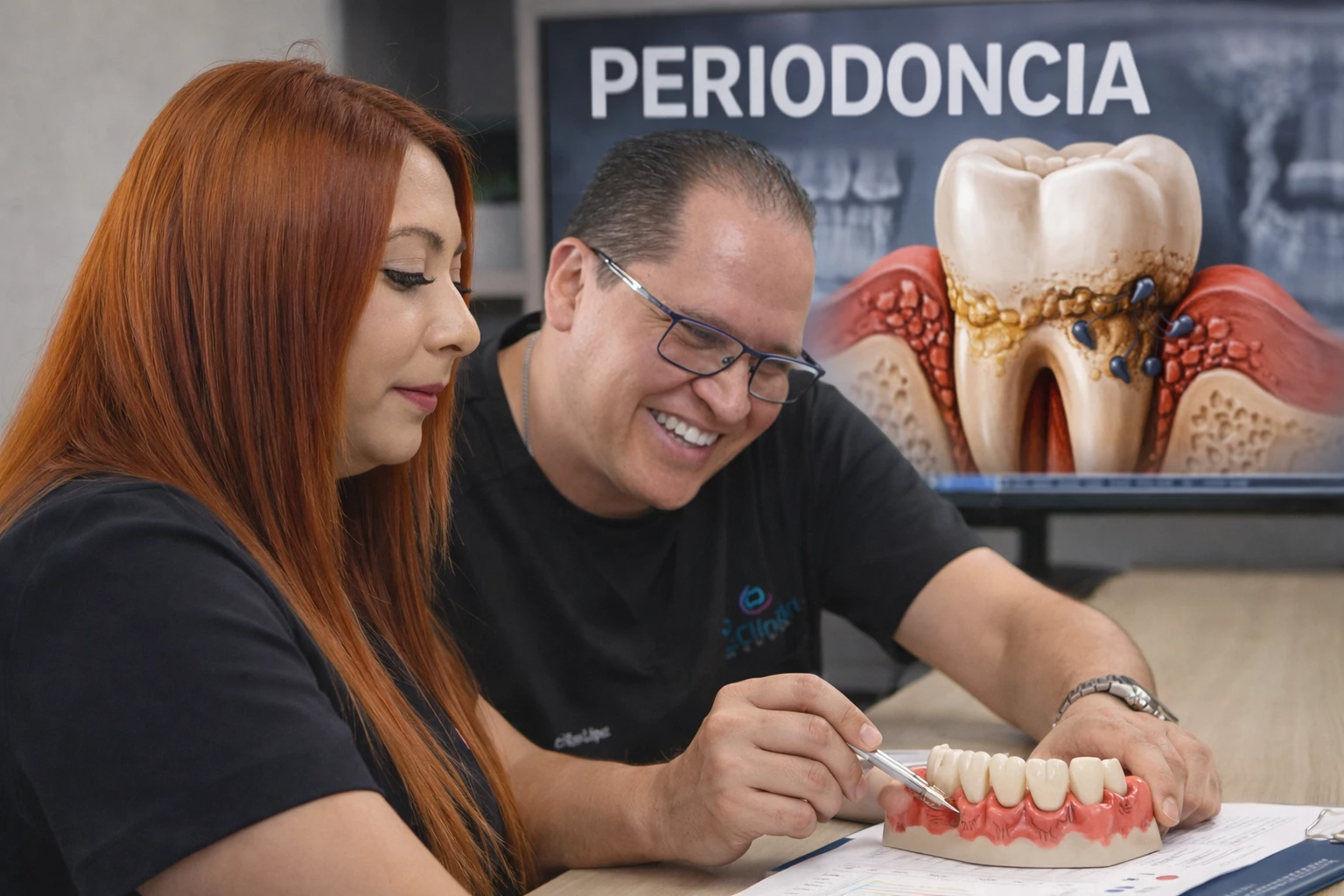
Periodontics is the dental specialty that diagnoses and treats diseases of the gums and the bone that supports the teeth. If your gums are bleeding, swollen, receding, persistent bad breath or you notice tooth mobility, it is not normal: it may be gingivitis or periodontitis. Taking care of it in time helps to preserve teeth, protect the bone, plan better implants and prevent a silent problem from turning into tooth loss or a more complex case.
Most patients do not seek a periodontist because “their gums hurt”. They seek help when there is already frequent bleeding, inflammation, sensitivity, gingival recession, loose teeth or fear of losing a tooth. That delay is precisely what makes a page like this so important: not only to explain what periodontics is, but to show why healthy gums are the foundation of a stable, functional and esthetically predictable mouth.
At La Clínica Dental, periodontics should not be understood as an isolated treatment. It should be integrated with diagnosis, rehabilitation, implants, dental esthetics and follow-up. That is why this guide is designed to answer in a clear way what a patient really wants to know: what he or she has, how serious it is, how it is diagnosed, how it is treated and what happens if it is not taken care of in time.
What is periodontics and what does a periodontist treat?
Periodontics is the dental specialty that deals with the prevention, diagnosis and treatment of diseases that affect the supporting tissues of the tooth: the gum, periodontal ligament and alveolar bone.
A periodontist treats problems such as:
- bleeding gums
- gingivitis
- periodontitis
- periodontal pockets
- gum recession
- bone loss around teeth
- tooth mobility
- periodontal maintenance
- gum health before implants, veneers or oral rehabilitation
- peri-implant problems in patients with implants
The difference between superficial dentistry and serious dentistry usually starts here: understanding that a mouth does not fail just because of a cavity or a broken tooth. Many times it fails because the biological support deteriorated over the years without the patient noticing it.
For patients who are already considering more complex treatments, this periodontal foundation should be assessed before moving on to procedures such as dental implants in CDMX, complete step-by-step rehabilitation or All-on-4 and All-on-6 in CDMX.
When does bleeding gums stop being “mild”?
It should never be standardized.
One of the most harmful ideas in oral health is to think that “if it bleeds a little, it is normal”. It is not. Bleeding is a sign of inflammation. In early stages it may correspond to gingivitis, but if the process continues, it can evolve into periodontitis and affect the bone that supports the teeth.
In addition to bleeding, other warning signs are:
- red or swollen gums
- persistent bad breath
- unpleasant taste sensation in the mouth
- gingival recession
- root sensitivity
- new spaces between teeth
- tooth mobility
- pain when chewing
- feeling that something “no longer feels the same” when the bite closes
| Symptom | What it may indicate | Level of alertness |
|---|---|---|
| Bleeding when brushing | Early gingival inflammation or gingivitis | High |
| Swollen or red gums | Inflammatory response to bacterial plaque and tartar | High |
| Persistent bad breath | Bacterial build-up and possible periodontal involvement | Medium-high |
| Gum recession | Loss of gingival tissue | High |
| Loose teeth | Loss of periodontal and osseous support | Very high |
| Chewing pain | Advanced inflammation, occlusal trauma or loss of support | Very high |
For users who come in with symptoms and don’t know if they need urgent care or a diagnostic evaluation, it’s a good idea to also link to what to expect at your first dental appointment.
Gingivitis vs. periodontitis: the difference that changes the prognosis
Not all bleeding gums mean the same thing. The big clinical difference is whether the problem is limited to superficial inflammation or if the destruction of the support has already begun.
Gingivitis
Gingivitis is the initial phase. There is inflammation, bleeding and redness, but there is not yet significant loss of supporting bone. In many cases it can be reversed with proper hygiene, professional cleaning and timely control.
Periodontitis
Periodontitis appears when inflammation progresses and affects deeper tissues. Periodontal pockets are formed, there may be attachment loss, recession, bone destruction and, in advanced stages, tooth mobility or loss.
| Condition | What does it affect? | Is it reversible? | Main risk |
|---|---|---|---|
| Gingivitis | Gum | Frequently yes | Progress if left untreated |
| Periodontitis | Gum, ligament and bone | It is controlled, not always completely reversed. | Loss of support and teeth |
Why do gums swell or bleed even if you brush daily?
Because brushing doesn’t always mean cleaning well.
Many patients brush every day, but do not completely remove plaque between teeth, at the gum margin or in hard-to-reach areas. When that plaque accumulates and mineralizes, it forms tartar. Tartar is not removed at home and favors the persistence of inflammation.
They can also have an influence:
- poor hygiene or poor brushing technique
- dental crowding
- defective restorations
- smoking
- diabetes
- hormonal changes
- oral respiration
- stress
- individual predisposition to inflammatory response
How is periodontal disease correctly diagnosed?
Periodontitis should not be diagnosed “at a glance” nor should it be resolved with a generic message of “you need a cleaning”. Serious diagnosis requires clinical and imaging integration.
Basic clinical evaluation
Must include:
- bleeding check
- measurement of periodontal pockets
- evaluation of shrinkage
- presence of plaque and tartar
- tooth mobility
- points of contact and spaces
- occlusion analysis
- medical history and habits
Imaging studies in periodontics: why they are key to more accurate diagnosis
In periodontics, imaging studies are not a decorative complement to diagnosis. They are a clinical tool to understand what is going on under the gum, to assess the actual bone support of each tooth and to make more accurate decisions.
When a patient presents with frequent bleeding, persistent inflammation, gingival recession, tooth mobility or suspected bone loss, visual examination alone is not enough. The periodontal evaluation should be supported by imaging studies to observe the bone level, root anatomy, possible bone defects and the relationship between the periodontal problem and other future treatments, such as dental implants in CDMX, comprehensive dental rehabilitation or more extensive esthetic procedures.
In practical terms, imaging studies help answer questions that the patient needs to understand clearly:
- Is there already bone loss?
- how advanced is the problem?
- Does the tooth still have a good prognosis?
- Is it possible to keep it or should we already think of another alternative?
- are there conditions that will affect a future implant or rehabilitation?
- Will the treatment be preventive, non-surgical or surgical?
Such diagnostic clarity completely changes the clinical conversation. An informed patient understands his problem better, accepts a logical plan more easily and avoids comparing his case with simplified treatments that do not correspond to his reality.
What imaging studies can be used in periodontics?
Not all patients require the same type of study. The choice depends on the clinical findings, the suspicion of bone loss, the complexity of the case and whether periodontal treatment needs to be integrated with other areas.
Digital panoramic radiographs
Digital panoramic radiographs provide an overview of the mouth and bony structures. They are useful as a starting point in patients who come in with a history of periodontal disease, tooth loss, previous treatment, generalized inflammation or a need for more extensive rehabilitation planning. If the patient wants to better understand how this resource works, they can review digital vs. conventional panoramic x-rays: benefits and how they work.
3D imaging and advanced studies in complex cases
When there is significant bone loss, implant planning, grafting, complex defects or the need for comprehensive rehabilitation, advanced dental technology allows you to better understand the anatomy of the case and plan with less uncertainty.
Intraoral scanning and digital case registration
Intraoral scanning does not replace clinical periodontal assessment and bone imaging, but it does improve case documentation, visual follow-up, patient communication and planning when periodontal health must be coordinated with rehabilitation, implants or esthetics.
It serves especially to show changes in dental architecture, wear, position, spacing and overall treatment context. It also makes it easier to compare the clinical evolution and helps to explain why a mouth with inflammation or loss of support should not be treated as if it were a purely esthetic case.
What information do these studies provide in a periodontal case?
Imaging studies can complement what is detected in the clinical examination. In a patient with periodontal disease, they can help to assess:
- height and quality of bone support
- distribution of bone loss
- presence of localized or generalized defects
- relationship between roots, bone and neighboring teeth
- general prognosis of compromised parts
- feasibility of preserving teeth before considering implants
- conditions for grafting, rehabilitation or periodontal surgery
In periodontics, treating without adequate clinical assessment and imaging may oversimplify a problem that actually compromises bone, tooth stability and future prognosis.
Imaging studies and planning for implants, grafts or oral rehabilitation
One of the biggest mistakes in dentistry is to plan implants or rehabilitation without first understanding the patient’s periodontal status. If there is active inflammation, bone loss or compromised support, the therapeutic decision changes.
Therefore, imaging studies are not only useful to confirm periodontal disease. They are also useful to decide if the case needs first gum control, maintenance, periodontal surgery, grafting or a more complex planning before rehabilitation.
How this technology improves planning without replacing clinical judgment
Digital imaging and complementary studies allow a better understanding of the level of bone support, document the case accurately and plan periodontal treatments, implants or rehabilitation with less uncertainty. They do not replace the specialist’s assessment, but they do improve the quality of the diagnosis and help to make more predictable decisions.
When this information is integrated with a complete clinical evaluation and with the patient’s functional context, periodontics is no longer seen as an isolated intervention and becomes the basis on which more stable treatments can be built, from gum control to procedures such as All-on-4 and All-on-6 in CDMX or the care and maintenance of dental implants and fixed prostheses in the long term.
| Treatment | When indicated | Primary Objective |
|---|---|---|
| Professional prophylaxis | Gingivitis or preventive control | Reduce plaque and superficial tartar |
| Scaling and root planing | Periodontal pockets or periodontitis | Decontaminate root surfaces |
| Adjunctive antimicrobial therapy | Selected cases | Support bacterial control |
| Periodontal surgery | Deep pockets or complex defects | Improve access, reduce pockets and stabilize tissues |
| Gingival grafting | Gingival retraction | Protect roots and improve stability/aesthetics |
| Periodontal maintenance | After disease control | Avoid relapses |
Is periodontitis completely cured?
The honest and clinically correct answer is this: gingivitis is usually reversible; periodontitis is usually controlled and stabilized, but does not always allow for complete recovery of lost tissue.
That doesn’t mean that the treatment “doesn’t work”. It means that the target changes:
- stop the progression
- reduce inflammation
- retain teeth
- to protect the remaining bone
- improve function and comfort
- reduce the risk of future complications
- better prepare other treatments
What happens if you do not treat periodontal disease in time?
Progression doesn’t always hurt at first. And that’s precisely why so many people are late.
When periodontal disease progresses unchecked, it can lead to:
- destruction of the supporting bone
- deeper periodontal pockets
- gum recession
- tooth mobility
- tooth spacing
- difficulty chewing
- abscesses or recurrent infections
- loss of parts
- more complex and costly rehabilitation cases
Periodontics and bone loss: the point at which waiting is no longer convenient
One of the biggest mistakes patients make is to seek help when they notice tooth mobility or feel that “the tooth is longer”. In many cases this means that the gum has receded or that the bone support has changed.
Periodontal bone loss not only compromises tooth stability. It also alters the prognosis of restorative treatments and, in some cases, makes it necessary to consider grafting procedures, rehabilitation or even implantological solutions if it is no longer possible to preserve certain teeth.
What is the relationship between periodontitis and heart problems?
This topic must be written with clinical precision, because authority is either gained or lost here.
The correct way to explain it is this:
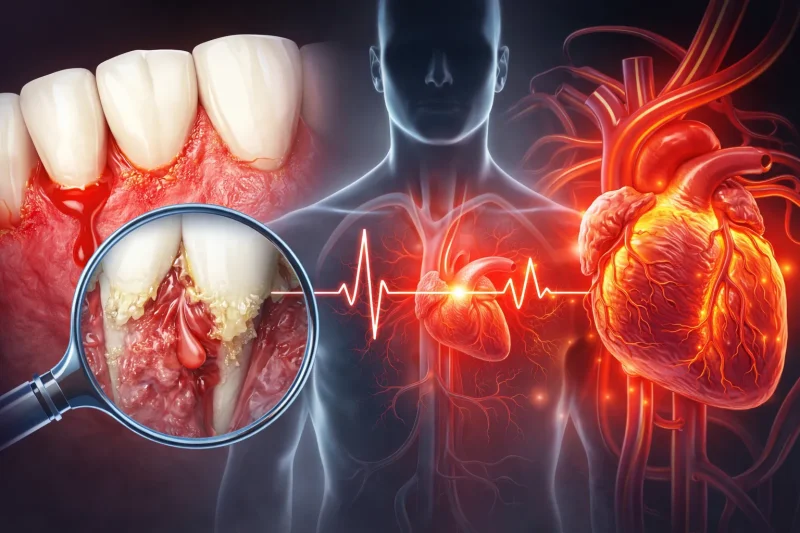
Periodontal disease should not be presented as the sole and direct cause of heart problems, but there is an important relationship between periodontitis and systemic inflammation, and this association has led to the study of its link with cardiovascular health.
What this means to a patient is not that “because you have swollen gums you will have a heart attack,” but that oral health is part of overall health and that ignoring chronic inflammation in the mouth is not a good medical decision.
Does periodontics also matter before implants, veneers or oral rehabilitation?
Yes, very much so.
Healthy gums are not an aesthetic detail. They are the biological basis for other treatments to have stability. If a patient wants to improve function, restore teeth or make an esthetic change, he or she must first check that the periodontal environment is adequate.
This is key before:
- dental implants
- fixed prostheses
- comprehensive rehabilitation
- smile design
- veneers
- extensive crowns
How often is periodontal maintenance needed?
Not all patients are at the same risk, and here is another point where the content should sound expert, not generic.
The ideal frequency depends on:
- history of gingivitis or periodontitis
- amount of plaque and tartar
- oral hygiene technique
- smoking
- diabetes
- depth of previous bags
- presence of implants or complex rehabilitations
- clinical response to treatment
A patient with a history of periodontal disease should not always follow the same schedule as someone who only comes in for routine preventive cleanings. That is why periodontal maintenance should be presented as part of the treatment, not as an optional service.
When should you visit a periodontist in CDMX?
You should seek periodontal assessment if you have one or more of these signs:
- frequent bleeding when brushing or flossing your teeth
- swollen or red gums
- persistent bad breath
- gingival recession
- root sensitivity
- tooth mobility
- sensation of pressure or discomfort when chewing
- history of bone loss
- desire to place implants or begin oral rehabilitation
- diabetes or smoking with symptoms of gingival inflammation
Also, if you are trying to decide between clinics, you may want to review a guide on how to evaluate a dental clinic in CDMX to understand why the difference is not only in the price, but in the diagnosis, traceability, materials and coordination between specialists.
Periodontics in CDMX with integral approach, digital diagnosis and long term vision.
Periodontics well done is not limited to control a punctual inflammation. It must be integrated with:
- digital diagnosis
- functional assessment
- rehabilitation planning
- dental conservation
- implants when they are really needed
- long-term follow-up
That is the angle that should make this page the cluster reference.
It’s not just a matter of saying “we treat gums”.
It is about making it clear that:
periodontics protects teeth, bone, implants, function and future stability.
What treatments are included in periodontics?
Periodontics is not a single treatment. It is a stepwise plan that depends on the diagnosis, the depth of the problem, the level of inflammation, bone loss and the clinical objective.
| Treatment | When indicated | Primary Objective |
|---|---|---|
| Professional prophylaxis | Gingivitis or preventive control | Reduce plaque and superficial tartar |
| Scaling and root planing | Periodontal pockets or periodontitis | Decontaminate root surfaces |
| Adjunctive antimicrobial therapy | Selected cases | Support bacterial control |
| Periodontal surgery | Deep pockets or complex defects | Improve access, reduce pockets and stabilize tissues |
| Gingival grafting | Gingival retraction | Protect roots and improve stability/aesthetics |
| Periodontal maintenance | After disease control | Prevention of relapses |
Is periodontitis completely cured?
The honest and clinically correct answer is this: gingivitis is usually reversible; periodontitis is usually controlled and stabilized, but does not always allow for complete recovery of lost tissue.
That doesn’t mean that the treatment “doesn’t work”. It means that the target changes:
- stop the progression
- reduce inflammation
- retain teeth
- to protect the remaining bone
- improve function and comfort
- reduce the risk of future complications
- better prepare other treatments
What happens if you do not treat periodontal disease in time?
Progression doesn’t always hurt at first. And that’s precisely why so many people are late.
When periodontal disease progresses unchecked, it can lead to:
- destruction of the supporting bone
- deeper periodontal pockets
- gum recession
- tooth mobility
- tooth spacing
- difficulty chewing
- abscesses or recurrent infections
- loss of parts
- more complex and costly rehabilitation cases
Periodontics and bone loss: the point at which waiting is no longer convenient
One of the biggest mistakes patients make is to seek help when they notice tooth mobility or feel that “the tooth is longer”. In many cases this means that the gum has receded or that the bone support has changed.
Periodontal bone loss not only compromises tooth stability. It also alters the prognosis of restorative treatments and, in some cases, makes it necessary to consider grafting procedures, rehabilitation or even implantological solutions if it is no longer possible to preserve certain teeth.
What is the relationship between periodontitis and heart problems?
This topic must be written with clinical precision, because authority is either gained or lost here.
The correct way to explain it is this:
Periodontal disease should not be presented as the sole and direct cause of heart problems, but there is an important relationship between periodontitis and systemic inflammation, and this association has led to the study of its link with cardiovascular health.
What this means to a patient is not that “because you have swollen gums you will have a heart attack,” but that oral health is part of overall health and that ignoring chronic inflammation in the mouth is not a good medical decision.
Does periodontics also matter before implants, veneers or oral rehabilitation?
Yes, very much so.
Healthy gums are not an aesthetic detail. They are the biological basis for other treatments to have stability. If a patient wants to improve function, restore teeth or make an esthetic change, he or she must first check that the periodontal environment is adequate.
This is key before:
- dental implants
- fixed prostheses
- comprehensive rehabilitation
- smile design
- veneers
- extensive crowns
How often is periodontal maintenance needed?
Not all patients are at the same risk, and here is another point where the content should sound expert, not generic.
The ideal frequency depends on:
- history of gingivitis or periodontitis
- amount of plaque and tartar
- oral hygiene technique
- smoking
- diabetes
- depth of previous bags
- presence of implants or complex rehabilitations
- clinical response to treatment
A patient with a history of periodontal disease should not always follow the same schedule as someone who only comes in for routine preventive cleanings. That is why periodontal maintenance should be presented as part of the treatment, not as an optional service.
When should you visit a periodontist in CDMX?
You should seek periodontal assessment if you have one or more of these signs:
- frequent bleeding when brushing or flossing your teeth
- swollen or red gums
- persistent bad breath
- gingival recession
- root sensitivity
- tooth mobility
- sensation of pressure or discomfort when chewing
- history of bone loss
- desire to place implants or begin oral rehabilitation
- diabetes or smoking with symptoms of gingival inflammation
Also, if you are trying to decide between clinics, you may want to review a guide on how to evaluate a dental clinic in CDMX to understand why the difference is not only in the price, but in the diagnosis, traceability, materials and coordination between specialists.
Periodontics in CDMX with integral approach, digital diagnosis and long term vision.
Periodontics well done is not limited to control a punctual inflammation. It must be integrated with:
- digital diagnosis
- functional assessment
- rehabilitation planning
- dental conservation
- implants when they are really needed
- long-term follow-up
That is the angle that should make this page the cluster reference.
It’s not just a matter of saying “we treat gums”.
It is about making it clear that:
periodontics protects teeth, bone, implants, function and future stability.
Frequently asked questions about periodontics
What is periodontics?
Periodontics is the dental specialty that prevents, diagnoses and treats diseases of the gums and bone supporting the teeth. Its goal is to control inflammation, preserve periodontal support and maintain long-term stability of teeth and implants.
Which specialist treats gums?
The specialist who treats the gums is the periodontist. He is trained to diagnose gingivitis, periodontitis, gingival recession, bone loss, periodontal pockets and other problems that affect the support of the teeth.
Is it normal for my gums to bleed when I brush?
No. Bleeding gums should not be considered normal. It is usually a sign of inflammation and may indicate gingivitis or periodontal disease. When bleeding is frequent, the correct thing to do is to have a periodontal evaluation and not just change toothbrushes or stop brushing.
What symptoms indicate periodontal disease?
The most frequent symptoms are bleeding, swollen gums, persistent bad breath, gingival recession, root sensitivity, tooth mobility, new spaces between teeth and discomfort when chewing. In some cases there is also a sensation of pressure, “receding gums” or teeth that feel longer.
What is the difference between gingivitis and periodontitis?
Gingivitis is the initial phase and mainly affects the gums. It usually presents with inflammation and bleeding, and many times it can be reversed with timely treatment. Periodontitis is a more advanced phase in which the bone and the supporting tissue of the tooth may already be affected. This difference changes the prognosis and the type of treatment required.
Can gingivitis be reversed?
Yes, in many cases gingivitis can be reversed if it is treated in time, the accumulation of plaque and tartar is eliminated and the patient improves his oral hygiene. The problem appears when the inflammation is maintained for a long time and progresses to periodontitis.
Is periodontitis completely cured?
Periodontitis is usually controlled and stabilized, but it is not always possible to completely recover all the lost tissue. The realistic goal of treatment is to stop progression, reduce inflammation, preserve teeth and maintain periodontal support as long as possible.
Can I lose teeth due to periodontal disease?
Yes, advanced periodontal disease can destroy tooth support and lead to tooth mobility or tooth loss. That is why early treatment is so important: the earlier it is diagnosed, the better the chances of preserving teeth and avoiding more complex treatment.
Why do my gums bleed if I brush every day?
Because brushing daily doesn’t always mean you’re removing plaque well. There may be buildup between teeth, near the gingival margin or in areas that are difficult to clean. Tartar, smoking, diabetes, defective restorations, dental crowding or insufficient hygiene technique can also play a role.
Do swollen gums always mean infection?
Not always, but they do mean that there is a problem that should be evaluated. In many cases the inflammation is related to bacterial plaque and gingivitis; in others it may be associated with periodontitis, local trauma, hormonal changes, oral respiration or systemic diseases. The important thing is not to normalize persistent inflammation.
What are periodontal pockets?
Periodontal pockets are deep spaces that form between the gum and the tooth when periodontal disease progresses. Their presence can hinder hygiene, favor bacterial accumulation and be a sign of loss of periodontal support.
What is periodontal bone loss?
Periodontal bone loss is the reduction of the bone that supports the teeth as a consequence of chronic inflammation associated with periodontitis. When it progresses, it can compromise dental stability, change the prognosis of the teeth and complicate future treatments such as implants or oral rehabilitation.
What studies are used to diagnose periodontitis?
Periodontal diagnosis combines clinical examination and complementary studies. It usually includes bleeding review, pocket measurement, retraction evaluation, tooth mobility and imaging studies to assess bone support and the complexity of the case.
Are imaging studies necessary in all cases?
Not in all cases with the same level of complexity, but they are very important when there is a suspicion of bone loss, tooth mobility, a history of periodontal disease, compromised teeth or the need to plan implants, grafts or rehabilitation. The image helps to better understand the real prognosis of each case.
What treatments are used in periodontics?
It depends on the diagnosis. Treatments may include professional cleaning, scaling and root planing, adjunctive antimicrobial therapy, periodontal surgery, gingival grafting and periodontal maintenance. Not all patients need surgery, but they do need a plan appropriate to the severity of their case.
What is scaling and root planing?
It is a deep periodontal treatment that seeks to eliminate plaque, tartar and bacteria adhered to the surface of the dental root. It is used when there is deeper inflammation or periodontal pockets and its objective is to reduce the bacterial load and promote tissue stability.
Does periodontitis always hurt?
No. That is one of its major problems. It often progresses silently or with very mild discomfort, so the patient does not consult until mobility, retraction, sensitivity or loss of support becomes more evident.
Does receding gums always need surgery?
Not always. Treatment depends on the cause, the degree of retraction, sensitivity, tissue stability and the functional or esthetic objective. In some cases it is sufficient to control inflammation and habits; in others a graft or more specific periodontal treatment may be advisable.
Does periodontal disease cause bad breath?
It can be a major cause of persistent bad breath. When there is bacterial accumulation, gingival inflammation or periodontal pockets, the patient may notice recurrent halitosis. If bad breath does not improve with regular hygiene, it is advisable to assess whether there is an underlying periodontal problem.
Does periodontics improve bad breath?
Yes, especially when the origin of bad breath is related to inflammation, bacterial plaque, tartar or periodontal disease. In those cases, treatment not only improves the gums, but also improves the overall oral environment.
What happens if I don't treat my gums in time?
The problem can progress. What starts as bleeding and inflammation can develop into periodontitis, bone loss, tooth mobility, separation between teeth and loss of teeth. In addition, an untreated case often requires more complex, longer and more costly treatments.
Can periodontal disease affect a dental implant?
Yes. The health of the gums and bone directly influences the environment in which implants are placed and maintained. A patient with active or poorly controlled periodontal disease may have a less favorable prognosis if they do not first stabilize inflammation and oral support.
Should the gums be treated before an implant?
Yes, before placing implants, the right thing to do is to evaluate and stabilize periodontal health. Healthy gums and adequate support improve planning, reduce risks and help the treatment to have a more stable biological basis.
Does periodontics also matter before veneers, crowns or smile design?
Yes, esthetic and restorative treatments work best when the periodontium is healthy. If there is inflammation, retraction or compromised support, stability and long-term outcome may be affected.
How often do I need periodontal maintenance?
It depends on your individual risk. Factors such as history of periodontitis, depth of previous pockets, smoking, diabetes, oral hygiene and presence of implants or complex rehabilitations all play a role. Periodontal maintenance should not be seen as an extra, but as part of the treatment.
Is a regular dental cleaning the same as periodontal treatment?
No. Routine preventive cleaning does not always solve a deeper periodontal problem. When pockets, persistent inflammation or loss of support are already present, a different treatment is usually required, with a more thorough assessment and specific follow-up.
Is periodontal disease related to diabetes?
Yes, diabetes and periodontal disease can influence each other. In patients with diabetes, gingival inflammation can be more difficult to control, and in patients with poorly controlled periodontal disease it can complicate the overall balance of the case. Therefore, both issues should be addressed in a coordinated manner.
Is there a relationship between periodontitis and heart problems?
There is an important association between periodontal disease and systemic inflammation, which is why its relationship with cardiovascular health is also being studied. The correct way to explain this is without exaggeration: it is not a matter of saying that all periodontitis causes a heart problem, but of understanding that oral health is part of general health.
How do I know if I need a periodontist or just a cleaning?
If you have frequent bleeding, persistent inflammation, recession, loose teeth, constant bad breath, root sensitivity or a history of bone loss, you need a more complete assessment than a regular preventive cleaning. In these cases it is advisable to check for periodontal disease and the actual level of involvement.
When should I see a periodontist in CDMX?
You should visit when you notice recurrent bleeding, swollen gums, receding gums, tooth mobility, persistent bad breath, discomfort when chewing or when you want to start implants, rehabilitation or esthetic treatments and need to confirm that the periodontal base is stable.
What if I already have bone loss?
It doesn’t automatically mean you will lose the tooth, but it does mean you need a serious periodontal evaluation. The key point is to determine how much support is left, whether the case can be stabilized and how that changes the overall treatment plan.
Is periodontics only for older adults?
No. Periodontal disease can appear at different times of life. Although certain problems are more prevalent with age, there are also young adults with gingival inflammation, loss of support or significant risk factors that require periodontal care.
What is the benefit of treating periodontal disease early?
Early treatment improves the prognosis, increases the possibility of preserving teeth, reduces the progression of the loss of support, facilitates other treatments and prevents a treatable problem from becoming a more complex rehabilitation.
Protect your gums before you lose support, bone or teeth.
If your gums are bleeding, swollen, receding or you feel tooth mobility, don’t let it go. An early periodontal evaluation allows you to identify the real cause, measure the level of involvement and define a clear plan to preserve teeth, protect the bone and correctly plan any future treatment. Schedule your periodontal evaluation in CDMX and know the real state of your gums before the problem becomes more complex.
Author:
Dr. Rosa María Moctezuma Lozano
National Autonomous University of Mexico
ID No. 1135288
Clinically reviewed and updated content for patient information guidance.
Last editorial revision: March 20, 2026.